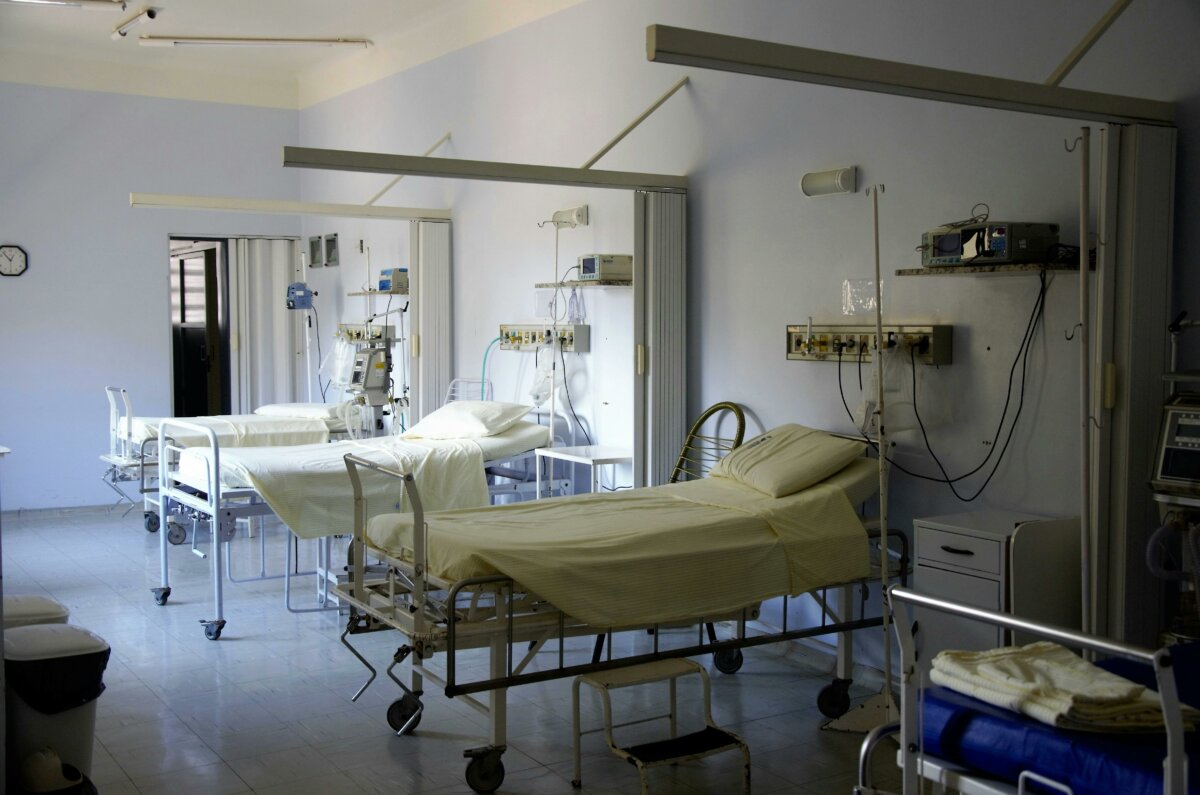
A report by SecondStreet.org reveals that at least 15,474 Canadians died in 2023-24 while waiting for surgeries or diagnostic scans.
The data presented in the 2024 edition of the Died on a Waiting List and collected through Freedom of Information (FOI) requests highlights significant gaps in healthcare delivery, with several jurisdictions either providing incomplete data or failing to track the issue entirely.
When accounting for provinces and regions that did not provide information, SecondStreet.org estimates the actual number of deaths could reach 28,077.
The findings span a range of medical services, including cancer treatments, heart operations, cataract surgeries, and MRI scans.
The report notes that patients died after waiting for periods ranging from less than a week to over 14 years. Ontario Health reported 378 deaths specifically linked to cardiac procedures.
Highlights:
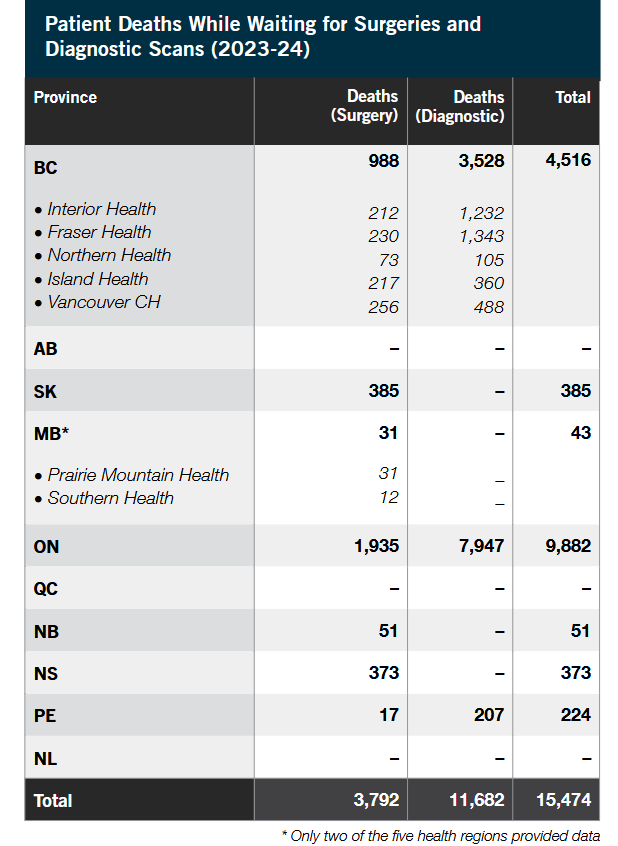
Credit: SecondStreet.org
- Ontario, Prince Edward Island, and British Columbia were the only jurisdictions that provided data on patients passing away while waiting for both surgeries and diagnostic scans.
- Quebec, Alberta, Newfoundland and Labrador, and most of Manitoba did not provide data.
- Saskatchewan, New Brunswick and Nova Scotia supplied information only on surgical waitlist deaths, excluding diagnostic scans.
- Based on available data, an estimated 28,077 Canadians died in 2023-24 while on healthcare waitlists.
- Since April 2018, 74,677 Canadians are reported to have died while waiting for medical care.
The report underscores systemic challenges in Canada’s healthcare system, often compared unfavourably to higher-performing universal systems in Europe. “Canadians pay high taxes, yet the system continues to fail,” said Harrison Fleming, Legislative and Policy Director at SecondStreet.org.
“When a restaurant fails a health inspection, the government shares the news publicly and sometimes notices are posted in the establishment’s windows for everyone to see,” said Colin Craig, SecondStreet.org President, criticizing governments for not proactively disclosing waitlist death data.
“But, when nearly 75,000 Canadians have died before getting the care they needed, governments don’t proactively disclose anything. Maybe it’s time for governments to hold themselves to the same standard they hold everyone else.”
The study was inspired by cases like Laura Hillier’s. Hillier, an 18-year-old cancer patient, died in 2016 after delays in scheduling a bone marrow transplant, despite having a donor lined up. Her case, which went viral on social media, underscores the urgent need for change.
According to the Fraser Institute, Canadian patients in 2024 waited an average of 30 months for treatment.
The report argues that comprehensive data collection and transparency are crucial steps toward addressing these systemic issues and saving lives.